Ailing Masses, Trailing Health Services And Healing Godmen of India
By Kandathil Sebastian
02 December, 2014
Countercurrents.org
There is a wide gap in accessing the health care services between various population groups in India. This is partly due to the failure of the health services system in meeting the expectations of the ailing masses in the backdrop of rapidly rising health care costs with no visible improvement in quality of health care services. This systemic failure has led to a widespread feeling of helplessness particularly among the rural masses of India while they deal with their health problems. They look for solutions from entities which are beyond the conventional providers such as quacks, sorcerers and godmen.
Most of those who flock to the godmen for miracle cures in India are from the groups of poor women, dalits and backward communities. They work as small farmers, agricultural laborers and artisans. They struggle hard at their work places under adverse weather conditions to produce food and other commodities for their urban counterparts. When they get sick, they have no one else to turn to except their God and these godmen who claim to have miracle cures for their ailments.
This essay examines the roots and nuances of this complex health seeking behavior of the ailing masses, the trailing health Services and the healing Godmen in India.
The Phenomenon of Healing Godmen
Look at the following three instances of ‘healing acts’ which takes place in the heartland of India. These are cited as examples and not to malign the religious beliefs of any community.
Around one lakh people from Maharashtra and the adjacent states visit one Nitin Maharaj’s ashram and temple on every Tuesday and Sunday. He gives a prasad made of crushed tomatoes harvested from the grounds around his temple. The believers who come to this temple are convinced about the miraculous healing powers of his prasad. There are many who could vouch for the prasad’s ability to cure a wide range of problems such as joint pain, head ache, tumors, diabetics, and even complications in the kidney. The temple has a filtration plant which supplies water for processing the tomato prasad. During the temple festival, up to a million people visit Nitin Maharaj’s ashram, leading to traffic chaos in the temple town. The Government makes elaborate security arrangements to control the crowd around the temple during festival days.
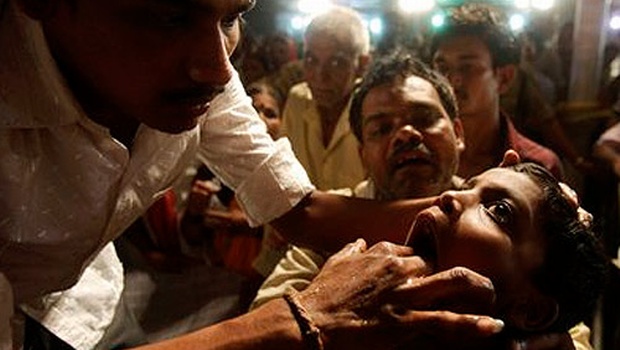
Every year, in the city of Hyderabad in neighboring Andhra Pradesh, at the onset of monsoon, thousands of people with asthma and respiratory infections stand in very long queues to meet members of the Bathini Goud family who distributes a fish prasad to asthma patients. The Bathini brothers first insert their prasad into the mouth of a live sardine fish which is about 2 to 3 inches long and then the live fish is slipped into the throat of the patient. The huge crowd which turns up to receive this miracle cure leads to serious chaos and even death due to stampede; the government arranges special police forces to manage the crowd at the site. It also arranges special trains for the patients to reach the venue on time.
Nirmal Darbar Trust in Jharkhand attracts thousands of people to attend healing sessions called ‘samaagam’ through advertisements in several TV channels. These sessions are conducted by one Nirmal Baba who was originally a Punjabi business man and a school dropout, who attained ‘nirvana’ after suffering two serious losses in bricks and clothes business. He declared himself as God earlier and now he claims to have cures for every ailment including asthma, diabetes, tuberculosis, hypertension, cancer, and even for AIDS.
India has many such individuals, families and trusts (which are managed like modern corporations) who claim to have miracle cures for all kind of ailments. Many of them are still at large though some of them like Baba Rampal and Asaram Bapu got arrested by the Indian police not for ‘healing diseases’ but for trying to expand their political clout through criminal activities. Many of these Babas and gurus claim to have special powers and that they have been anointed by the God to heal the afflictions of humanity.
They often have a very huge fan following in the rural heartland of India. They are omnipresent and they travel to many places to conduct mass healing sessions in emotionally charged gatherings. Such healing individuals who claim shamanic powers are not limited to Hinduism only, they present in all other religions including Islam and Christianity. These godmen like the shamans of yester years play multiple roles as a magician, medicine person, miracle-worker, healer, priest, mystic and master of all spiritual energies and enjoy the company of powerful business tycoons and politicians.
There are many social scientists who tried to analyze and explain why India has so many godmen who had successfully set up their spirituality enterprises, networked with powerful politicians and enjoyed a huge fan following among the masses. Life and its myriad unknown puzzles and unexplored conundrums always gave Indian gurus and godmen ample opportunities to indulge in numerous intellectual philosophical discourses and to attract people from faraway places who are in their ardent quest for meanings and answers, and interested in knowing multiple interpretations and answers to their existential dilemmas. But rallying behind them in large numbers to find cures for the health problems is not necessarily due to their intellectual journey to explore domains where science could not venture and therefore this phenomenon needs further analysis.
In the absence of a working health services system in the rural areas, many of the godmen are doing a boundless service to the masses. Health is believed to be a state of complete wellbeing and not mere absence of diseases. It indicates a balanced co-existence of a sound mind in a sound body in a sound environment. When this equilibrium of inter linkages among body, mind and community is affected by an external agency or organism humans get sick. Restoring the lost equilibrium is a psychosomatic process which involves participation of patient’s body, mind and the community within which the patient lives.
An attitude of optimism, hope in getting back to health, faith in oneself, faith in the healer and his techniques, faith in one’s God etc. have always helped the healing processes to become faster. Faith in God and belongingness to a community which has strong supportive bonds have also been said to have decisive impact in the healing process. Faith healing along with medicines and in some cases without medicines has been reported in modern times too. Quiet often the negative results of faith healing are ‘explained away’ by attributing them to personal defects.
The phenomenon of godmen is not confined to the north Indian states where the health services are very weak, but even in states like Kerala where a robust and efficient health care services system exists. Thousands of people from Kerala rush to ‘divine healing centres’ set up around the clout of healing Christian priests who are believed to have the ability to perform miracles, exorcise demons and heal afflictions. The rising cost of health care in the backdrop of the state’s epidemiological transition due to which the state has progressed from a dominant communicable diseases profile to a dominant lifestyle related diseases profile made the people bewildered and stranded. This situation has provided a fertile soil for evangelic faith healers. Godmen continue to flourish in soils where access to health care is limited, irrespective of the affluence of people living in an area.
The phenomenon of godmen who uses ‘faith healing’ techniques is neither limited to a particular time like that the one we live currently nor to a particular country like India. The relative failure of the US health care system to provide affordable care to its comparatively marginalized citizens led to the growth of faith healers in the fringe groups of Christianity. They have also accepted faith healing as an acceptable and integral part of their worship and religious practices. There is enough justification to include American evangelists such as Kenneth Hagin, Kenneth Copeland, Charles Parham, Rex Hubbard, Benny Hinn, and Oral Roberts into the group of godmen who are in the profitable business of healing using almost the same techniques and processes used by Indian Godmen.
All of them advertise their miracles through TV and social media. Like Nirmal baba of India, the American evangelists also believe that health and illness are direct results of either ‘purity’ or ‘sin’ in one’s life and give opportunities to confess their sins and suggests remedies to ‘purify’ the ‘soul’ and ‘body’ of their patients.
It does not matter even if the evidence of healing offered by these Godmen does not stand up to scientific scrutiny. Their followers continue to believe in the testimony of those who got healed, though their healing is only a subjective experience. Critics of faith healers are usually dealt with personal attacks and they are blamed of not having enough faith. Defense of faith healers is usually based on ‘insider/outsider separation’. They gather support from members of their mother religion by crying ‘attack on their holy faith by nonbelieving outsiders’. They survive as medical science too does not have answers to all the questions about health, diseases and the multiple ways through which healing takes place.
The Situation of the Ailing Masses
Millions of rural people in India succumb to deaths due to diseases such as malaria, tuberculosis, kala azar and Japanese Encephalitis that could have been avoided with basic medication or treatment. Most of these preventable deaths in villages are due to infections of communicable, parasitic and respiratory diseases. Deaths in villages from conditions like nutritional deficiencies or perinatal deaths are also avoidable if they could have accessed some kind of affordable, basic health care at the right time.
Around 40% of the rural morbidity in India is thanks to water born infectious diseases. These diseases are (1) of the gastrointestinal tract - such as diarrhoea, amoebiasis, typhoid fever, infectious hepatitis, worm infestations and poliomyelitis, (2) carried in the air through coughing, sneezing or even breathing -such as measles, tuberculosis, whooping cough and pneumonia, or (3) the difficult ones - like malaria, filariasis and kala-azar.
About 100 million people get diarrhoea and cholera every year. There are 12 million tuberculosis cases currently in India with 1.2 million cases added every year. Around 37, 000 cases of measles are reported every year. About 2.3 million episodes and over 1000 malarial deaths occur every year in India. An estimated 45 million people are carriers of microfilaria. Around 1.2 million cases of leprosy exist in India with 500, 000 cases being added every year. More than 85% of rural children are undernourished and around 150, 000 of them die every year.
In theory, the government provides some kind of health services - a three tier structure of health care consisting of Community Health Centres, Primary Health Centres and Subcentres is set up for the rural areas. But whatever limited services exist in the rural areas are either nonfunctional, dysfunctional, or are with extremely ‘poor quality’. Most often the service providers, especially doctors are not present in the rural facilities. A 2004 study by Bannerjee and others in the rural areas of Rajasthan have found that 45% of the doctors are absent from the Primary Health Centres and 56% of sub-centers remains closed maximum of the times. The situation is not very different even today also.
India has just six doctors and nine hospital beds for every 10,000 of its people, compared to 14 doctors and 30 hospital beds in China. About 75% of health infrastructure, medical manpower, and other health resources are concentrated in urban areas where 28% of the populations live in villages. A recent survey of 15,000 households across 12 states, conducted by IMS Institute for Healthcare Informatics in India noted that about half the people in India and over three-fifths of those who live in rural areas have to travel beyond 5 km to reach a healthcare centre. The survey further points out that the availability of healthcare services is skewed towards urban centers with these residents, who make up only 28% of the country's population, enjoying access to 66% of India's available hospital beds, while the remaining 72%, who live in rural areas, have access to just one-third of the bed.
Villages in the heartland of India are inhabited by poor landless laborers, small holders, and artisans. They spent their money mostly on food and some money on clothing and housing. Considering their ‘subsistence existence’, spending money on health care is indeed a luxury to them. Most of them could not afford to buy health care from the urban centers just because they are poor. Therefore in case of extreme illnesses, the rural masses turn to the private providers for which they have to borrow money from the money lenders.
Many studies (including those done by the NSSO and the NCAER) have shown that medical treatment is the most important cause of rural indebtedness, next only to dowry in the rural India. Those who are indebted and those who are unable to afford a loan finally turn to quacks, sorcerers and godmen. Not only in remote rural and tribal areas but also in urban slums, the phenomenon of godmen is rampant and these godmen meet a felt need of these ailing masses.
Roots of Massive Ailments and Trailing Health Services in Rural India
The roots of widespread Ill Health and the trailing health services can be traced back to colonialism and the colonial models of health services development which was followed by various governments in independent India. Large scale commercial exploitation (mainly mining of minerals to sustain the industrial revolution of Europe and colossal cutting of trees to make battle ships and railway sleepers) affected India’s ecology. The commercial forestry not only disrupted the hydrology of forests by reducing the biomass production but also affected the health of the tribal population whose sustenance and survival was dependent of these forests.
For the smooth passage of raw materials, the British not only constructed railways but also made huge canals. Malaria followed these canals during 1840 -1890. The development paradigm of colonialism continued in the independent India leading to several other water born infections. Large scale irrigation projects brought malaria and filariasis; pesticide use has produced a drug resistant strain of malaria, the ditches, gutters and culverts dug during the construction of roads created breeding places for mosquitoes.
Unfavorable trade practices and demand for excessive land revenue led to decline in the living standards, low income levels, rural distress and growth of urban slums. The socioeconomic, cultural and political onslaughts of colonialism endangered access to healthy and nutritious food, clean air and water, nutritious vegetation, and healthy life styles of the masses.
Colonialism destroyed the balance between people and their environment including coping mechanisms such as indigenous healing traditions. Lack of patronage resulted in the gradual decline of indigenous medical traditions. The training of medical practitioners during the colonial period was mainly to provide subordinates to the Europeans in the Indian Medical Service. Medical education was a neglected area after the independence too. Today only 193 of India’s 640 districts have medical colleges.
There is a serious national shortage of health workers especially in rural areas. Though the immediate reason for this shortage is the reluctance of the medical professionals to serve in rural areas, the fundamental reason of it is the failure of the Indian medical establishment to mold and orient young professionals to serve in the rural areas not only by inculcating values of serving the needy masses in the rural areas but also by providing them required amenities in those areas. The need to recover the money invested by the professional is also a compelling reason to stay away from non-profitable rural areas.
The technology in which a medical professional was trained is not available in rural facilities. Their training is overly focused on technology and dependent on diagnostics and therefore it cannot be extrapolated to rural areas. The Government has also failed to provide basic infrastructure and incentive structure, and a job environment and modes of recognition for doctors and other health workers to be motivated enough to do their work in rural areas.
The health services in India during the colonial period was molded essentially to serve the Indian Civil Services, the army and the European population living in India; it did not respond to the health needs of the masses. It was racially skewed and focused on curative services; urban hospitals and dispensaries were established mainly to cater the needs of the British and Indian elites. The preventive and sanitary measures were available only to European troops and European quarters in towns.
The health services infrastructure which the Independent India created, especially the primary health centres that were set up to cater the health care needs of the rural poor were burdened with family planning work, especially in achieving targets of sterilization. Health care was commodified mainly by the influence of the pharmaceutical companies who operated with a perspective in which healthcare was equated with the supply of their products. Privatized Healthcare was looked up while the government health care was discredited due to poor quality and obsession with birth control.
In the independent India, we had undue focus on vertical programming and campaigns around certain diseases which has been singled out. Vertical programmes for small pox, filariasis, tuberculosis, leprosy and HIV/AIDS have taken most of our personnel and resources. At the end of these campaigns, some diseases offered slow and persistent resistance (e.g. leprosy), some have developed new facets for which new solutions were to be found (e.g. drug resistant malaria), and some are prevalent in small pockets (e.g. schistosomiasis).
All these factors precipitated a ‘disease-oriented cure system’ rather than a ‘health-oriented care system’. Today we have a highly selective, institutionalized, centralized, and top down health care services system which treats people as objects rather than subjects. It failed to address the needs of the rural poor and indigenous people.
Going beyond the Godmen
The problem of poor access to health care by the masses is well documented by researchers umpteen times. The policy and program measures to deal with this issue are also known to experts. What we lack is the political will and guts to implement certain drastic measures. Today we are left with two options in front of us. We can either continue to leave the health care of the masses to shamans, sorcerers and godmen; and when they rally behind their miracle cures, we can blame them for their ignorance and superstitious habits and plan media campaigns to educate them! Or we can take bold steps to ensure universal access to health care.
In addition to priority allocations of resources and personnel to rural areas we need to strive for setting up total health systems designed around the life patterns of the rural population to support their health care needs based on the principles of equity and their active participation. Many primary causes of ill health are based on factors such as poverty, deprivation and environmental abuse. The health support systems of the poor are clean water, air, forests and land. Threat to these resources is the root cause of their ill health. The current policies governing the natural resource use encourage chemical inputs based agriculture, commercial forestry, mining and are creating serious problems to the livelihood, lifestyles and health of not only those who are directly affected but also to the future generations.
Investing in God and godmen may help the ruling regimes to contain dissent of the masses for a short while. But investing in health and welfare of the masses will help in establishing longstanding peace and happiness to everyone.
Kandathil Sebastian is a Development Consultant and Public Health Researcher. He is also the Author of two novels – ‘Dolmens in the Blue Mountain’ and ‘Wisdom of the White Mountain (forthcoming)’.
.
Comments are moderated

